The Purpose of this Information
This information is being provided to you in order to prepare you to make decisions about your own health care. If you should ultimately decide that surgery is the best treatment option for you, this section will help you understand what happens during an anterior cervical discectomy and will help you prepare for your role in the healing and recovery process. Read it thoroughly and answer the questions before making your final decision about your treatment options.
The Health Care Team’s Role
The duty of your health care team is to:
- evaluate your condition
- establish a diagnosis
- present the various treatment options
- offer a specific treatment recommendation
- provide you with the information you need to make a decision; and then
- support you in the decision you make
The Patient’s Responsibilities
You are the only one who can decide to have surgery. It is important that you take ownership of this decision, recognizing the limitations your particular physical condition places on the potential success of each of the treatment options.
If you choose to have surgery, your physical condition and your mental attitude will determine your body’s ability to heal. You must approach your surgery with confidence, a positive attitude, and a thorough understanding of the anticipated outcome. You should have realistic goals – and work steadily to achieve those goals.
The decision to have or not to have surgery includes weighing the risks and benefits involved. You will make the final decision, so ask questions about anything you do not understand.
Since medical care is tailored to each person’s needs and differences, not all information presented here will apply to the patient’s treatment or its outcome. Seek the advice of your physician and other members of the health care team for specific information about the patient’s medical condition.
Anatomy of the Back
The spinal column, or backbone, consists of 33 bones (vertebrae) and can be divided into five segments (Fig. 1A). The uppermost 24 vertebrae are separated from one another by fibrous cartilage pads, called intervertebral discs (Fig. 1B), which allow the spine to bend and act as shock absorbers during activity. In the lowest part of the spine, the vertebrae are naturally fused to form the sacrum and the coccyx (tail bone).
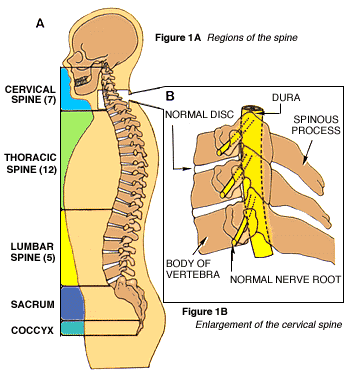
Protruding from the back of each block-like vertebral body is an arch of bone that helps to form the large, vertical spinal canal, which surrounds the spinal cord and nerve bundles (Fig. 1C, below). A fluid-filled protective membrane, the dura, covers the contents of the spinal canal from where the cord begins at the base of the brain to where it ends (in a bundle of nerve fibers known as the cauda equina).
A pair of spinal nerves branches at each vertebral level (one to the left and one to the right), providing sensation and movement to all parts of the body. Three large bone processes arise from the vertebrae’s arch-one to each side (transverse) and one straight toward the back of the body (spinous). Strong ligaments and muscles attached to the vertebrae both support the spine and further protect the delicate spinal cord and nerves inside.
Anterior Cervical Discectomy
What is it?
Anterior cervical discectomy is an operation performed on the upper spine to relieve pressure on one or more nerve roots, or on the spinal cord. The procedure is explained by the words anterior (front), cervical (neck), and discectomy (cutting out the disc).
Why is it done?
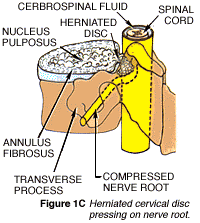
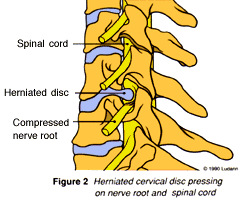 Neck and arm pain, among other symptoms, may occur when an intervertebral disc herniates. This happens, either suddenly with injury or slowly over time, when some of the disc’s jelly-like center (the nucleus pulposus) bulges or ruptures through its tough, fibrous outer ring (the annulus fibrosus) and presses on a nerve (Fig 1C, above).
Neck and arm pain, among other symptoms, may occur when an intervertebral disc herniates. This happens, either suddenly with injury or slowly over time, when some of the disc’s jelly-like center (the nucleus pulposus) bulges or ruptures through its tough, fibrous outer ring (the annulus fibrosus) and presses on a nerve (Fig 1C, above).
When a disc ruptures in the cervical spine, it puts pressure on one or more nerve roots (often called nerve root compression) or on the spinal cord, as seen in (Figure 2). This pressure causes symptoms in the neck, arms, and even legs. Further pressure may be caused by rough edges of bone, called bone spurs, that naturally build up around some herniated discs.
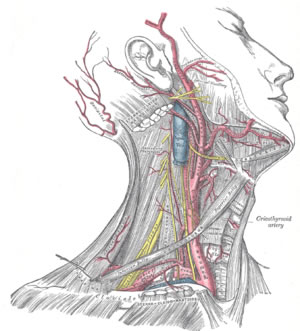 In this operation, the cervical spine is reached through a small incision in the front of your neck. After the soft tissues of the neck are separated, the intervertebral disc and bone spurs are removed. The space left between the vertebrae may be left open or filled with a small piece of bone. In time the vertebrae may fuse, or join together.
In this operation, the cervical spine is reached through a small incision in the front of your neck. After the soft tissues of the neck are separated, the intervertebral disc and bone spurs are removed. The space left between the vertebrae may be left open or filled with a small piece of bone. In time the vertebrae may fuse, or join together.
If used, the pre-formed bone graft may be obtained from a bone bank. It will not be rejected by your body, because it is avascular (contains no blood cells). In some circumstances, or if your surgeon prefers, the bone graft might instead be removed from your own hip through a second incision.
What happens afterwards?
Successful recovery from anterior cervical discectomy requires that you approach the operation and recovery with confidence based on a thorough understanding of each process. Your surgeon has the training and expertise to correct physical defects by performing the operation; he and the rest of the health care team will support your body’s efforts to heal its damaged tissues. Full recovery will also depend on you having a strong, positive attitude, setting small, realistic goals for improvement, and working steadily to accomplish each goal.
The Operation
Incision:
Surgery for anterior cervical discectomy is performed with the patient lying on his or her back. A small incision is made in the front of the neck, to one side (Fig. 2).
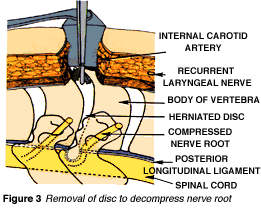
Exposure and removal of the herniated disc
After a retractor is used to pull aside fat and muscle are pulled, the disc is exposed between the vertebrae. Part of the disc is removed with a forcep (Fig. 3).
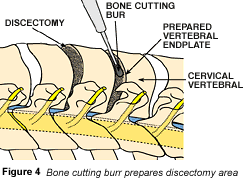
The surgical drill is then used to enlarge the disc space (Fig. 4) making it easier for the surgeon to empty the interverterbral space fully and remove any bone spurs. Afterwards, only a single ligament separates the surgical instruments from the spinal cord and nerve roots.
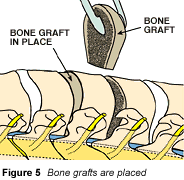
Placement of the bone graft
The bone graft is placed in the disc space, where it will begin to fuse the vertebrae it lies between (Fig. 5)
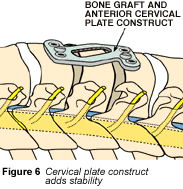
Adding Stability: Fusion
In fusion, your doctor joins (fuses) the vertebrae above and below the removed disk. Fusion is done with a bone graft, but occasionally metal plates are added. Metal plates add stability to the cervical spine and aid in the healing process. (Fig. 6)
Incision Closure
The operation is completed when the neck incision is closed in several layers. Unless dissolving suture material is used, the skin sutures (stitches) or staples will have to be removed after the incision has healed. Click on the picture to enlarge it.
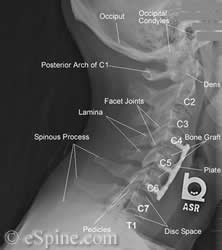
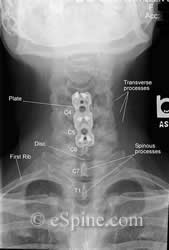
X-Rays
X-rays are taken to verify the position of the instrumentation. Below is a patient with a two level cervical fusion.
Click on the X-rays to enlarge them.
Risks
Certain risks must be considered with any surgery. Although every precaution will be taken to avoid complications, among the most common risks possible with surgery are: infection, excessive bleeding (hemorrhage), and an adverse reaction to anesthesia.
Other risks possible when anterior cervical fusion include: stroke, injury to the recurrent laryngeal nerve, which causes hoarseness and may or may not be permanent; and injury to the involved nerve root(s) or the spinal cord, both of which can cause varying types and degrees of paralysis.
Clinical experience and scientific calculation indicate that, in general, surgical risks are limited; however, surgery is a human effort. Unforeseen circumstances can complicate any surgical procedure and lead to serious or even life-threatening situations. Although such complications are rare, you should feel free to discuss the question of risk with your doctor.
Hospital Recovery
Pain
It is normal to have some pain after the operation, especially in the incision area. This does not mean that the procedure was unsuccessful or that your recovery will be slow. Pain in the neck or arms also is not unusual, caused by inflammation of the previously compressed nerve. It will slowly lessen as the nerve heals. Medication will be given to control pain. Moist heat and frequent repositioning may also help.
Numbness
Tingling sensations or numbness are often the last symptoms to disappear. Numbness that lingers in parts of the arm or fingers usually is no cause for worry and should gradually go away.
Physical activity
You may move about in bed and rest in any comfortable position when you have recovered from anesthesia. Walking may begin within several hours. The easiest way for you to get out of bed is to raise the head of the bed as far as it will go, and then swing your legs to the floor. Avoid pulling up from a flat position with the overhead trapeze.
Your physician may order a cervical collar for you to wear whenever you are up and about. Your nurse will explain its proper use.
Gradually increase the amount of walking you do each day. Since it may at first be painful, try making short trips. Begin with a trip to the bathroom, then to the door, and later out into the corridor. Sitting and standing also require a gradual pace. If discomfort occurs, change positions frequently.
Hygiene
Unless instructed otherwise, you may take a shower the day after surgery. This will help you feel better and should be done with the dressing left in place to protect the incision. Your nurse will change the dressing afterwards.
Nutrition
Intravenous (I.V.) fluids will be ordered during the early recovery period and continued until you can tolerate regular liquids without nausea or vomiting. Your diet will then be adjusted back to normal as your appetite returns. Constipation will be treated with laxatives and a diet of whole grain cereals, fruits, and fruit juices.
Emotional changes
You may feel discouraged and tired for several days after surgery. These feelings may be your body’s natural reaction to the cutback of extra hormones put out to handle the stress of surgery. Although emotional let-down is not uncommon, it must not be allowed to get in the way of the positive attitude essential to your recovery and the return to normal activity.
Discharge from the hospital
The hospital stay for patients undergoing anterior cervical discectomy usually lasts several days. Length of stay will be determined by your progress and by the amount of comfort and help available to you at home.
Home Recovery
Physical activity
Daily walking is the best exercise during recovery. Try to increase your distance a little each day, setting a pace that avoids fatigue or severe pain. Climb stairs when you feel able.
Sexual relations may be resumed during the recovery period, but positions that strain the neck or cause pain should be avoided.
“Listen” to your body. Discomfort is normal while you gradually return to normal activity, but pain is a signal to stop what you are doing and proceed more slowly.
Working
Your doctor will help determine when you can return to work and with what limitations. If a work release is necessary, it will be given to you during a postoperative visit.
Driving
Drive a motor vehicle only when you have recovered full coordination and are experiencing minimal pain. Do not drive after taking pain medication.
Medication
You should gradually use less pain medication while recovering at home. This can be accomplished by increasing the amount of time between taking pills, then by reducing the number taken each time. Some discomfort and pain in the neck and arm(s) can be expected until the inflammation and nerve sensitivity have ended. Heat, exercise, massage, and short rest periods will also help relieve pain.
Hygiene
If the skin sutures were removed before your discharge from the hospital, it is not necessary to keep the incision covered. Unless instructed otherwise, you may take a daily shower or tub bath, which will help you feel better. Let the water run over the incision, but do not scrub or rub over it. Pat it dry. After bathing, massage lotion over your tightened neck muscles.
If you notice increased redness, swelling, or any drainage around the incision after leaving the hospital, notify your physician.
Nutrition
A well-balanced diet is necessary for proper healing. Include foods from each basic food group: dairy products, meats, vegetables, and fruits. Since you will be less active during recuperation, avoid rich, heavy foods, and those high in calories but low in nutrients.
Healing and Recovery
Healing
Healing is the body’s natural process of restoring its own tissues to a normal or nearly normal state. Although healing may be improved by general good health, proper nutrition, rest, and physical fitness, it will occur without your having to work at it.
Recovery
Recovery is the process during which you work to become well. It requires a gradual but persistent effort to increase physical strengths and minimize weaknesses. Concentrate on improvement, not on what symptoms remain. This focus on progress, combined with the constant effort to improve, maintains the positive attitude that will speed your return to improved daily activity.
Making Sure You Understand…
Test your knowledge of anterior cervical discectomy by answering these questions.
- What is a herniated disc? How can it cause neck and arm pain?
- Why may a bone graft be used? Why isn’t it rejected by your body?
- Why is there still pain in the neck or arms after surgery-sometimes even temporarily worse than before?
- After the operation, how soon may you return to everyday physical activity?
- When should you wear the cervical collar? Why?
- What will help relieve pain besides medication?
- What is the difference between healing and recovery? How does a positive attitude affect each?
- Are you comfortable with your understanding of the risks of this procedure? Do you realize the part human effort plays in its expected outcome?
- Are you a member of the health care team?
Glossary
Because medical terms and concepts can often seem overwhelming, especially during times of stress, a few key definitions are repeated here.
Anterior – front; for this topic; anterior refers to the convenient approach used by the surgeon to reach a cervical disc through the front of the neck
Cervical spine – refers, in general, to the neck; the uppermost region of the backbone, including: the first seven vertebrae, the nerve elements (spinal cord and nerve roots) inside them, and all supporting structures that join them together
Discs – fibrous cartilage pads that lie between the spinal vertebrae; each is made up of two parts: a jelly-like center (the nucleus pulposus) that loses moisture with age, and a tough outer ring (the annulus fibrosus) that can split with age or injury
Discectomy – cutting out (-ectomy) of an intervertebral disc
Graft – a piece of tissue transplanted to replace one that’s damaged or diseased; in this case, a bone graft may be used to fill the emptied intervertebral disc space
Herniated disc – the rupture of the center of an intervertebral disc through its fibrous outer ring and causes compression of the spinal cord or nerve roots; also called ruptured disc or (incorrectly) slipped disc
The human body is an intricate network of interrelated systems. Each system functions on its own but is also influenced by and dependent upon the others. When illness or injury occurs, it disrupts the function of one or more of these systems.
Surgery is a human effort made to correct one system’s malfunction, but it will affect all others. Because of this complex interrelationship, surgical outcomes cannot be predicted.
When recovery is possible, it occurs as a combination of the surgeon’s effort, the patient’s faith, and a positive acceptance of the outcome.